January 1, 2000, dawned with promise in America. The Y2K computer bug many feared would bring widespread disruption mostly fizzled out. Among the bright spots that would follow that year was a landmark announcement from the Centers for Disease Control and Prevention: Measles was eliminated in the United States.1
It was news to celebrate. Before the measles vaccine’s wide rollout in 1963, the viral respiratory illness was contracted by 3 million to 4 million people each year, causing as many as 500 deaths, 4,800 hospitalizations, and 1,000 cases of encephalitis.1 To get to elimination—which the CDC defines as the “absence of continuous disease transmission for greater than 12 months”—children began receiving a second dose of the measles vaccine, which is now standard protocol.
But today, the news again is sobering. In 2018, there were 17 reported measles outbreaks affecting 372 people. (The CDC defines an outbreak as three or more cases.) By mid-February 2019, there were 127 reported cases, with reported outbreaks in Washington, Texas, and New York, and cases reported in California, Colorado, Connecticut, Georgia, Illinois, Kentucky, and Oregon.2
Why the unwelcome resurgence of this contagious virus? The CDC says there are two leading causes:3
- Travelers are bringing the virus to the United States from countries experiencing an unusually high number of measles cases. Today, these countries include England, France, Germany, India, the Philippines, and Vietnam.
- The virus is spreading through communities whose residents are unvaccinated.
Nurses are often the first medical professionals to see patients presenting with measles symptoms, and the CDC has specific information and requirements for healthcare professionals. Here are vital facts every nurse should know:
Clinical Features
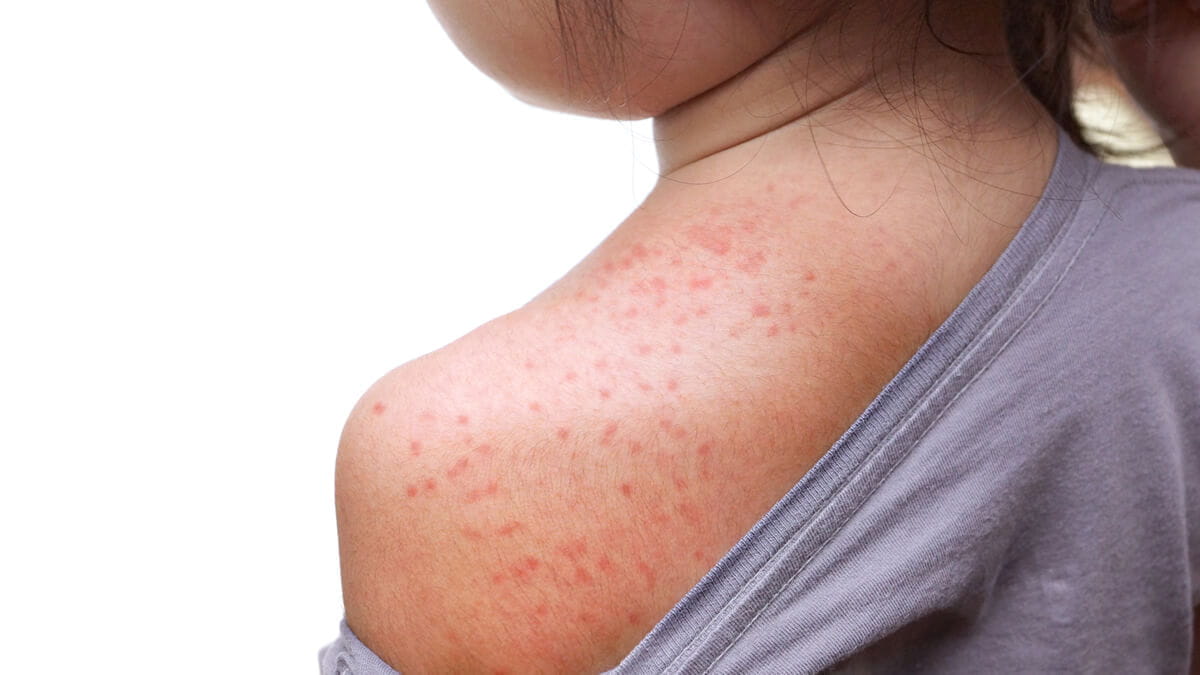
“Measles is an acute viral respiratory illness,” the CDC explains. “It is characterized by a prodrome of fever (as high as 105 degrees Fahrenheit) and malaise; cough, coryza, and conjunctivitis … [and] a pathognomonic enanthema (Koplik spots) followed by a maculopapular rash. The rash usually appears about 14 days after a person is exposed. The rash spreads from the head to the trunk to the lower extremities. Patients are considered to be contagious from four days before to four days after the rash appears. Of note, sometimes immunocompromised patients do not develop the rash.”4
Complications
The CDC says common complications include otitis media, bronchopneumonia, laryngotracheobronchitis, and diarrhea.4
Transmission
“Measles is one of the most contagious of all infectious diseases; approximately 9 out of 10 susceptible persons with close contact to a measles patient will develop measles,” the CDC says. “The virus is transmitted by direct contact with infectious droplets or by airborne spread when an infected person breathes, coughs, or sneezes. Measles virus can remain infectious in the air for up to two hours after an infected person leaves an area.”4
Diagnosis
“Healthcare providers should consider measles in patients presenting with febrile rash illness and clinically compatible measles symptoms, especially if the person recently traveled internationally or was exposed to a person with febrile rash illness,” the CDC advises. “Healthcare providers should report suspected measles cases to their local health department within 24 hours.”4
Isolation
“Infected people should be isolated for four days after they develop a rash; airborne precautions should be followed in healthcare settings. Regardless of presumptive immunity status, all healthcare staff entering the room should use respiratory protection consistent with airborne infection control precautions (use of an N95 respirator or a respirator with similar effectiveness in preventing airborne transmission),” the CDC says.4
Treatment
“There is no specific antiviral therapy for measles. Medical care is supportive and to help relieve symptoms and address complications such as bacterial infections,” the CDC says.4
U.S. Surgeon General Jerome Adams has joined the CDC, health departments, doctors, nurse practitioners, and others in urging parents to vaccinate their children, and for unvaccinated adults to follow suit. “It’s up to all of us, together, to protect the health of our communities,” Adams says.5
Advance Your Career in Nursing to Meet Today’s Challenges
A Master of Science in Nursing can prepare you for a leadership role in any of the dynamic fields in nursing. And choosing an online nursing school is a smart move for working professionals. You can log in and complete coursework on a timetable that works for you.
The ever-changing world of healthcare offers nursing careers for all interests and ambitions. Pick an MSN program that provides the specialization you seek to achieve your goals. Options may include public health nursing, nursing education, family nurse practitioner, and adult-gerontology primary care nurse practitioner. Choose a path that will position you to make a difference in the lives of patients and their families, and in doing so, build healthier communities.
Walden University is an accredited institution offering a Master of Science in Nursing (MSN) degree program with eight specializations. Expand your career options and earn a degree online in a convenient, flexible format that fits your busy life.
1 Source: www.cdc.gov/measles/about/history.html
2 Source: www.cdc.gov/measles/cases-outbreaks.html#outbreaks
3 Source: www.cdc.gov/measles/about/faqs.html
4 Source: www.cdc.gov/measles/hcp/index.html
5 Source: www.youtube.com/watch?v=Y0qcmB51qTk&feature=youtu.be
Walden University is accredited by The Higher Learning Commission, www.hlcommission.org